New joint guidance
The guidance on reflective practice for doctors and medical students has been developed jointly by Academy of Medical Royal Colleges, the UK Conference of Postgraduate Medical Deans (COPMeD), the General Medical Council (GMC) and the Medical Schools Counsel (MSC).
The guidance considers why reflecting on experiences, both positive and negative, is vital for being an effective doctor and for the wider system, and includes techniques for reflection, as well as considering some of medico-legal questions on reflection.
Clare Owen, assistant director at MSC, said:
“Medical students learn that education is a continuum, not just through further training but through learning that is self-directed and drawn from everything they do in practice.
Being a doctor means having the ability to reflect on practice and the decisions made each day. This guidance will be an invaluable tool for medical schools as they train students in this key skill.”
Becoming a reflective practitioner
Reflecting helps individuals and teams to demonstrate insight and identify learning opportunities to improve future practice. It’s an important skill to develop when entering clinical settings and allows the quality and safety of patient care to be constantly reviewed and improved.
The guidance encourages doctors and students to reflect on a variety of situations, such as after a clinical interaction with a patient on a placement and even after you’ve read an interesting piece of research or an article. Complaints and compliments are a good source of material for reflection as these often highlight areas that could benefit from improvement or where you are able to do things particularly well. As important as individual reflection is team reflection where colleagues can learn from each other to improve practice in their organisation.
Reflection in action
The reflective practitioner – guidance for doctors and medical students suggests ways to approach reflection constructively including, the What? So what? Now what? framework, published by the GMC.
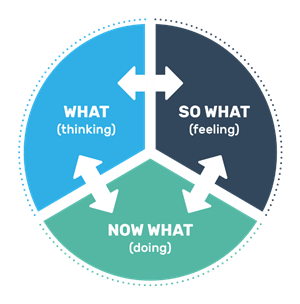 What? focuses on thoughts at the time of an experience. It explores thought processes when a particular action or decision was taken and how those may have impacted on actions and feelings.
What? focuses on thoughts at the time of an experience. It explores thought processes when a particular action or decision was taken and how those may have impacted on actions and feelings.
For example, “What was I thinking when I took the actions or made the decision that I did”
So what? involves considering the significance of what happened as well as the values and feelings at the time of and prompted by the experience, and why these may influence future learning or actions.
For example, “How did I feel at the time of and after the experience, why was it important?”
Now what? looks at the processes and opportunities that can help learning from the experience and identifying future actions, reflection on those actions, and how to use these to develop further.
For example, “What can I learn from or do differently next time”
There are lots of techniques to explore. Find out more about the ‘WHOA!’ model of reflection developed by Warwick Medical School or writing a reflective diary.
Read more in The reflective practitioner – guidance for doctors and medical students.
For medical students and doctors, reflecting on your practice is vital to ensure you review the decisions you make and learn from them. Reflecting allows health professionals to identify gaps in their knowledge or weaknesses, where further training and professional development may benefit to them and their patients.
However, it’s also important to reflect on the things we do well or where we have received positive feedback from our colleagues or patients. This helps to maintain good practice and may provide opportunities to impart our knowledge on colleagues or help an organisation improve its systems.
Where medical students and doctors have been subject to an investigation, for example by their medical school, hospital or the GMC, the MDU encourages reflection and insight so there is confidence an individual has learned from an incident and has considered what they would do next time, if they found themselves in the same position again. Doing so may reassure investigators that the individual has proactively remediated and no further action is necessary.
As well as reflecting on incidents, it’s also important to keep a reflective log of any professional development you engage in, such as conferences, lectures and teaching sessions. Rather than record what was discussed or presented, make a note of what you have learned from the session and how this will impact on your practice in future. This is an important part of a health professional’s appraisal and revalidation.
Dr Kathryn Leask
Medico-legal adviser
Dr Kathryn Leask
Medico-legal adviser
BSc (Hons) MBChB (Hons) LLB MA MRCPCH FFFLM RCPathME DMedEth
Kathryn has been a medico-legal adviser with the MDU since 2007 and is a team leader, trainer and mentor in the medical advisory department. Before joining the MDU, she worked in paediatrics gaining her MRCPCH in 2002 and holds a CCT in clinical genetics. She has an MA in Healthcare Ethics and Law, a Bachelor of Law and a Professional Doctorate in Medical Ethics. She is also a fellow of the Faculty of Forensic and Legal Medicine and has previously been an examiner and deputy chief examiner for the faculty. Kathryn is currently a member of the faculty’s training and education subcommittee and a member of the Royal College of Pathologists (medical examiner).
See more by Dr Kathryn Leask